Dr Isolde Hertess assesses and treats suitable patients for gynaecomastia on the Gold Coast. Planning is based on your symptoms, your anatomy, and the likely cause, because treatment options can differ depending on whether the main issue is gland tissue, fatty tissue, or both.
View our gallery of past patient results
See our gallery of real patient results from past surgeries performed by Dr Isolde Hertess. Patient results should not be viewed as a reflection of results other patients may experience
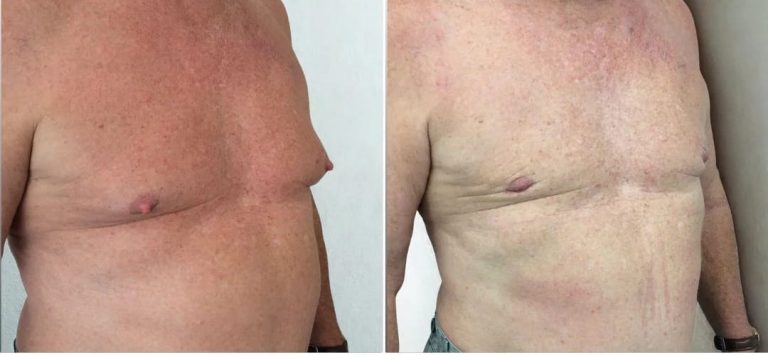
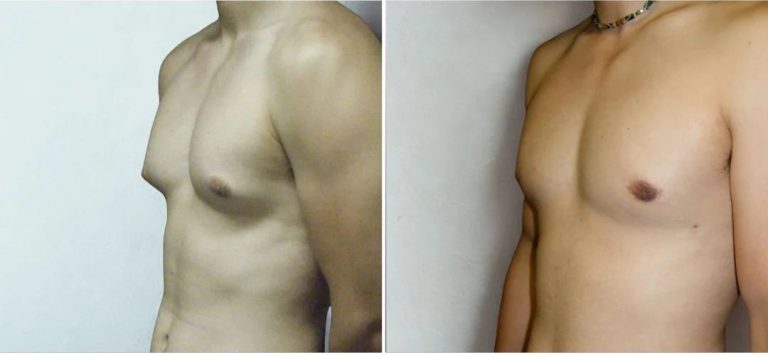
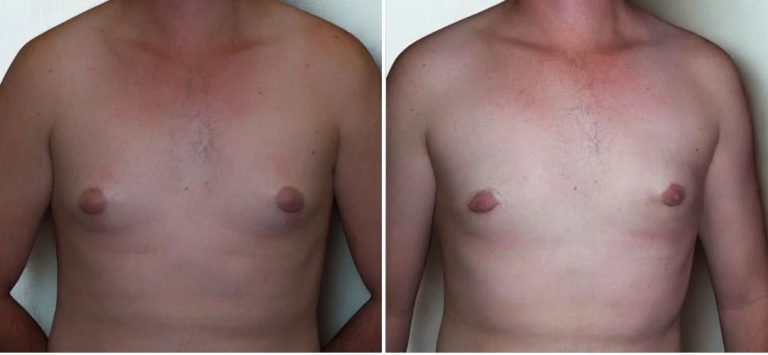
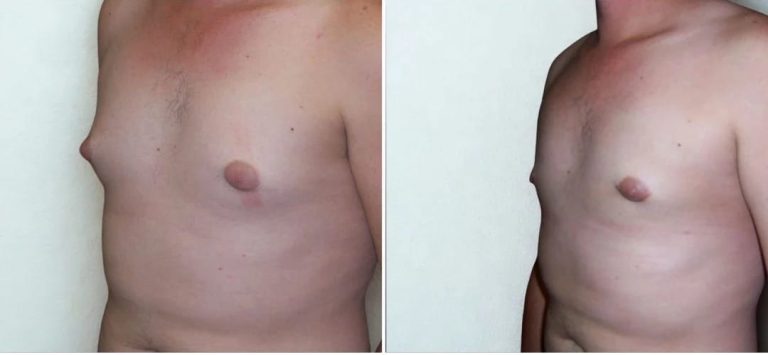
Disclaimer: The outcomes shown are only relevant for that patient and do not necessarily reflect the results other patients may experience. Results may vary due to many factors, including the individual’s genetics, diet, and exercise.
What Is the Difference Between Gynaecomastia and Fat in the Chest?
This is an important part of the assessment because it affects treatment.
- Gynaecomastia refers to glandular (breast) tissue. It is often described as firmer tissue under the nipple.
- Fat in the chest can look similar, but it is mainly fatty tissue rather than gland tissue. This is also known as pseudogynaecomastia.
- A combination is also common, where there is both gland tissue and fatty tissue.
A physical examination helps clarify what is contributing most to the appearance and feel of the chest.
Why Patients Develop Gynaecomastia
Gynaecomastia can occur for different reasons, and sometimes more than one factor is involved. Common contributors include:
- Hormone changes
- Certain medications
- Use of anabolic steroids or hormone products
- Some recreational drugs
- Alcohol use
- Medical conditions that affect hormone balance
- Weight changes, which can also increase fatty tissue in the chest
If gynaecomastia is new, painful, one-sided, or associated with a lump, discharge, or skin changes, medical assessment is important to rule out other causes.
More than 30 years of experience, Female support Dr Isolde Hertess – Plastic Surgeon
Offering a female perspective, with more than 30 years of experience in plastic and reconstructive surgery. Dr. Hertess is dedicated to providing patients with information, support, and guidance to help them make informed decisions about their surgical options.

How Gynaecomastia Is Assessed
Assessment usually includes:
- A medical history, including medicines and supplements
- A discussion about when the change started and whether it has progressed
- A physical examination of the chest and surrounding tissues
- Discussion of whether blood tests or imaging are appropriate, depending on the clinical situation
This assessment is important because it helps clarify whether surgery is the most suitable approach or whether medical management and monitoring should be considered first.
Treatment Options for Gynaecomastia
Treatment depends on the cause, severity, tissue type, and how long it has been present. Options may include:
Observation and Medical Review
In some cases, especially if gynaecomastia is recent, a period of observation may be recommended. If a medicine or hormone-related factor is suspected, medical review may be needed before considering surgery.
Surgery
Surgery may be considered when gynaecomastia is long-standing, does not settle, or causes ongoing concern. Surgical options depend on what is found during assessment and may include:
- Liposuction: If fatty tissue is a major component, liposuction may be used to remove fat and change the chest contour. Liposuction uses small incisions and a thin tube to remove fat.
- Excision of Gland Tissue: If firm gland tissue is present, removal of gland tissue may be needed. This is often done through an incision around the edge of the areola.
- Skin Tightening or Skin Removal: If there is significant skin laxity, additional skin tightening or removal may be discussed. This can involve additional scars, and whether it is needed depends on your skin quality, the amount of tissue removed, and your chest shape.
During your consultation at the Gold Coast, Dr Isolde Hertess will explain what options are likely to suit your situation and what can reasonably be expected from surgery.
Recovery After Gynaecomastia Surgery
Recovery depends on what is done during the surgery. Swelling and bruising are common in the early weeks, and you will usually need to reduce activity for a period, especially heavy lifting and upper body strain. You may also be advised to wear a compression garment, depending on your surgical plan and how healing is progressing.
Follow-up appointments are an important part of care because they allow healing to be checked and any concerns to be addressed early. Your chest can continue to change as swelling reduces and the tissues soften, so it can take time before the final shape becomes clear.
Gynaecomastia Surgery Risks
All surgery carries risks. The risks vary depending on whether liposuction, gland removal, or skin removal is required.
General surgical risks may include:
- Bleeding or haematoma
- Infection
- Fluid collection (seroma)
- Blood clots
- Wound healing problems
- Scarring that may be more noticeable than expected
- Anaesthetic risks
Procedure-specific risks may include:
- Changes in nipple sensation (temporary or permanent)
- Chest contour irregularity or asymmetry
- Skin changes
- Delayed healing around the areola
- Pigment changes around the areola
- Persistent breast tissue if the gland tissue is not fully addressed
- The need for further surgery in the future
These risks should be discussed in the context of your medical history and the planned approach.

